Arthritis
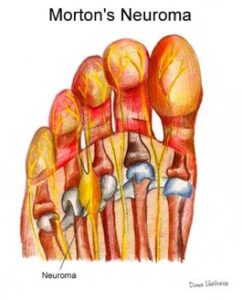
Morton’s Neuroma
Arthritis is a group of inflammatory conditions involving damage to the joints of the body.
There are many different forms of arthritis. The most common form, osteoarthritis (degenerative joint disease) is commonly a result from trauma to the joint, infection, poor bio-mechanics, age, hereditary and many other causes. Other forms of arthritis include rheumatoid arthritis, psoriatic arthritis, and related autoimmune diseases.
The major complaints by individuals who have arthritis are joint pain, swelling and stiffness. The pain from arthritis occurs due to inflammation that occurs in and around the joint.
Classification
Primary forms of arthritis:
- Osteoarthritis
- Rheumatoid arthritis
- Septic arthritis
- Gout and pseudo-gout
- Juvenile idiopathic arthritis
- Still’s disease
- Ankylosing spondylitis
Secondary to other diseases:
- Ehlers-Danlos Syndrome
- Sarcoidosis
- Psoriatic arthritis
- Reactive arthritis
- Haemochromatosis
- Hepatitis
- Wegener’s granulomatosis (and many other vasculitis syndromes)
- Lyme disease
- Inflammatory bowel disease (Including Crohn’s Disease and Ulcerative Colitis)
Osteoarthritis
Osteoarthritis is the most common form of arthritis. It can affect both the larger and the smaller joints of the body. The disease is most commonly acquired from daily wear and tear of the joint. Family history also plays a role in developing osteoarthritis. Osteoarthritis typically affects the weight bearing joints like the feet, knees and hips.
Osteoarthritis, like rheumatoid arthritis, cannot be cured, but one can prevent the condition from worsening. When it deals with the foot and ankle, orthotics, alterations in shoe gear, and many braces may help a significant amount. Cortisone injections are also sometimes helpful and warranted. Alterations in athletics impact sports and anti-inflammatory medications are widely used by individuals with osteoarthritis. Weight loss is also helpful to improving symptoms and preventing progression. When the disease is advanced and the pain is continuous, surgery may be an option. Surgery is based on failing conservative care, the amount of joint damage, age of the patient, overall recovery demands. Many common surgeries for arthritis range from cleaning up the joint/spurs (cheilectomy), to implants and fusions.
Rheumatoid arthritis
Rheumatoid arthritis is a disorder in which the body’s own immune system attacks its own tissues and joints. The attack is not only directed at the joint but often too many other parts of the body. In rheumatoid arthritis, most damage occurs to the joint lining and cartilage. Rheumatoid arthritis affects joints in the feet, fingers, wrists, knees and elbows. The disease is bilateral (affects both sides of the body) and symmetrical which can lead to severe deformity if not treated. Rheumatoid arthritis begins most often between the ages of 40 and 60, but can occur at any age. In children, the disorder can present with a skin rash, fever, pain, disability, and limitations in daily activities. With earlier diagnosis and aggressive treatment, many individuals can lead a respectable quality of life. The drugs to treat rheumatoid arthritis range from non-steroidal, anti-inflammatories, corticosteroids to other immunosuppresants given intravenously. Surgery may be required to realign, fuse or replace joints.
Gouty arthritis
Gout is caused by deposition of uric acid crystals in the joint, causing inflammation. There is also an uncommon form of gouty arthritis caused by the formation of rhomboid crystals of calcium pyrophosphate known as pseudogout. In the early stages, gouty arthritis usually occurs in one joint, but with time, it can occur in many joints including tendons and acute flares are extremely painful and crippling. In our practice gout is a very common problem. This is usually treated by a variety of medications (indomethacin, colchicine, or steroids) for acute gout attacks. Sometimes intra-articular injections, immobilization, alteration in diet, avoidance of alcohol, and narcotics are also needed. If the cause of an acute gouty attack is from a medication, then alteration in this medication may be needed. For the chronic stages of gout, treatment greatly changes. Diet, foot support, and a lowering uric acid medication is common to prevent further joint deterioration and pain. Surgery is usually avoided due to possibility of increasing or worsening a gout attack.
Diagnosis
Diagnosis is made by clinical examination, and may be supported by other tests such as radiology and blood tests, depending on the type of suspected arthritis. All types of arthritis potentially feature pain and pain patterns may differ depending on the specific arthritis and the location. Gout is associated with acute, severe pain with joint swelling, redness and warmth to the affected area.
Elements of the history of the disorder guide the diagnosis. Important features are speed and time of onset, pattern of joint involvement, symmetry of symptoms, early morning stiffness, tenderness, or locking with inactivity, aggravating and relieving factors, and other systemic symptoms.
Prevention
While neither rheumatoid arthritis nor osteoarthritis can be completely prevented, one can reduce the risks by becoming physically active, participating in physical therapy, losing weight and eating healthier. All individuals who have pain in the joints should seek early diagnosis because the earlier the treatment is started, the better the prognosis. Gout attacks can be prevented by understanding your family history and predisposing factors with medications and diet.

